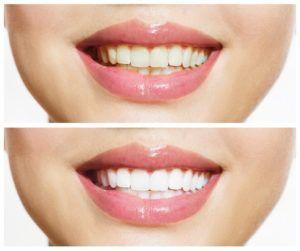
Radiating Confidence with Cosmetic Dentistry in Clearwater, FL
Your smile is your most powerful accessory. It speaks volumes before you’ve even uttered a word. In Clearwater, Florida, there’s
Comparing Dental Implants and Dentures: What’s Best for You?
Ensuring you have a healthy and beautiful smile is a significant aspect of your overall well-being. However, life can sometimes
Can All This Holiday Stress Affect Your Oral Health?
The holiday season is a time filled with joy, celebration, and a whole lot of stress. Between shopping for the
Holiday Oral Health Guide: Sugar, Teeth, and Tips – Clearwater, FL
The holiday season is a time of joy and celebration, but it can also be a challenging time for maintaining
Top Questions to Ask Your Sedation Dentist in Clearwater, FL
Prepare for your sedation dentistry experience by knowing the crucial questions to ask your dentist in Clearwater, FL. Sedation dentistry
Recovering After Sedation Dentistry Session in Clearwater, FL
Experience a smooth and stress-free recovery process following your sedation dentistry session in Clearwater, FL. Good news for those who
Tips on Choosing the Right Sedation Dentist in Clearwater, FL
Discover the ultimate guide to choosing the perfect sedation dentist in Clearwater, FL. Don’t let dental anxiety hold you back
Cost of Sedation Dentistry in Clearwater, FL: Is It Worth It?
What is the Cost of Sedation Dentistry? The cost of using general anesthesia for sleep dentistry ranges from $400 to
How Sedation Dentistry in Clearwater, FL Can Help with Special Needs Patients
When it comes to dental care, some individuals require extra support and attention to ensure a relaxed and anxiety-free experience.
Sedation Dentistry in Clearwater, FL: A Solution for Sensitivity
Are you tired of feeling discomfort and pain every time you indulge in your favorite cup of coffee or savor
The Connection Between Oral Health and Overall Wellness
When it comes to your well-being, did you know that your oral health plays a significant role? Many individuals mistakenly
Managing Dental Phobia with Sedation Dentistry in Clearwater, FL
iscover how sedation dentistry in Clearwater, FL can help overcome your dental phobia! Don’t let fear hold you back from
Sedation Dentistry in Clearwater, FL for Wisdom Teeth Removal
Looking for a stress-free solution to wisdom teeth removal? Discover the wonders of sedation dentistry in Clearwater, FL. At our
The Importance of a Comfortable Dental Experience
If the mere thought of visiting the dentist fills you with dread, rest assured that you’re not alone. Dental anxiety
What Happens During a Sedation Dentistry Procedure in Clearwater, FL?
Interested in what happens during a sedation dentistry procedure in Clearwater, FL? Experience a behind-the-scenes tour of the process and
Sedation Dentistry in Clearwater, FL vs. Traditional Dentistry
Making decisions about dental care can be overwhelming, but we’re here to help. At our practice, we understand that every
The Role of Sedation Dentistry in Pediatric Dentistry
Understanding Sedation Dentistry for Children Dental visits can be overwhelming for kids, causing anxiety and fear. Sedation dentistry helps children
How to Prepare for Your Sedation Dentistry Appointment in Clearwater, FL
Welcome to our dental practice where we prioritize your comfort and well-being! Don’t let anxiety overshadow your upcoming dental appointment
Exploring the Types of Sedation Used in Dentistry
Are you feeling anxious about visiting the dentist? You’re not alone. Dental anxiety affects millions of people worldwide, turning even
Common Misconceptions About Sedation Dentistry
Don’t let misconceptions hold you back from the best dental care in Clearwater, FL. Sedation dentistry is a valuable tool
Who Can Benefit from Sedation Dentistry?
At our practice, we believe that sedation dentistry is not limited to individuals with dental phobias or anxiety. It presents
Is Sedation Dentistry Safe? What You Need to Know
When dental appointments evoke fear or extensive procedures are necessary, sedation dentistry comes to the rescue, providing a smoother and
Understanding the Different Levels of Dental Sedation
Set sail on a voyage through the realms of dental sedation. Explore the diverse levels of sedation and unearth the
The Benefits of Sedation Dentistry: Overcoming Dental Anxiety
If you are tired of feeling anxious and fearful about visiting the dentist, discover how the revolutionary technique of sedation
Enjoy Your Favorite Foods With Dental Implants
The ramifications you can suffer due to tooth loss are numerous … remaining teeth can shift creating a malocclusion; difficulty
Are Dental X-Rays Safe? – Clearwater Dentistry
YES! X-rays have been used in dentistry for a long time, and the amount of radiation has significantly decreased with
The Link Between Dental Hygiene And Your Overall Health – Clearwater Dentistry
When patients of Andrew J. Holloman, DDS & Associates hear any mention of oral or dental hygiene, they probably think
Radiation And The Safety Of Dental X-Rays – Clearwater Dentistry
It is not uncommon to be concerned about your safety when you have dental X-rays performed. Putting on a heavy
Warning Signs Of Impacted Wisdom Teeth – Clearwater Dentistry
When your wisdom teeth start to emerge it can definitely be painful, but it can be even worse if your
Enjoy Your Favorite Foods With Implant Dentistry In Clearwater FL
The ramifications you can suffer due to tooth loss are numerous … remaining teeth can shift creating a malocclusion; difficulty
What’s The Connection Between Gum Disease And Diabetes? – Clearwater Dentistry
People who have diabetes are usually familiar with many of the other health risks they face, including damage to the
How Do I Handle My Child’s Dental Emergency? – Clearwater Dentistry
With children undergoing developmental dental changes and engaging in rough-and-tumble activities, dental emergencies can sometimes arise. If your child knocks
Clearwater FL Family Dentist Discusses Sedation Dentistry
If your child is particularly nervous about having work done at the dentist, or if she requires extensive treatment such
Good Oral Health Habits When You’re Pregnant – Clearwater Dentistry
Dr. Andrew Holloman and our team at Andrew J. Holloman, DDS & Associates will tell you that good oral health
Diabetes And Dental Care – Clearwater Dentistry
When most people think of complications of diabetes, they think of an increased risk of blindness, limb amputation, heart disease,
February Is Heart Month – Clearwater Dentistry
The American Academy of Periodontology stresses the importance of good oral health since gum disease may be linked to heart
The Connection Between Your Mouth And Your Heart – Clearwater Dentistry
At Andrew J. Holloman, DDS & Associates, we know your dental health is closely connected to your overall health. We
Choose Chocolate On Valentine’s Day – Clearwater Dentistry
From a student handing out sweets for her classmates to an older married couple exchanging boxes of candy, Valentine’s Day
Valentine’s Day History – Clearwater Dentistry
Valentine’s Day is best known as a celebration of love in all its forms. Pink hearts, red roses, and cute
Are You At Risk For Sleep Apnea? – Clearwater Dentistry
If you are one of the more than 12 million North Americans who suffers from sleep apnea, Dr. Andrew Holloman
Should I Use Mouthwash? – Clearwater Dentistry
Mouthwashes are commonly used as a part of a daily oral care regimen. Not only do they freshen breath, but
Clearwater FL Emergency Dentist Helps You Be Prepared
A dental emergency can be stressful and even frightening. However, if you are prepared, you’ll be able to act more
Tooth Discoloration: Common Causes And What You Can Do To Stop It – Clearwater Dentistry
Looking back at childhood photos, you may notice picture after picture of yourself with a mouthful of shiny white teeth.
Proper Flossing Techniques – Clearwater Dentistry
Of all the dental hygiene techniques you can use at home to promote clean teeth and good oral health, flossing
March Is National Nutrition Month! – Clearwater Dentistry
While you don’t have to wait to start eating right, March is the month the Academy of Nutrition and Dietetics
Easing The Teething Blues – Clearwater Dentistry
Every moment of your baby’s first year of life is precious, since every day your child grows a little, develops
Are Your Teeth Ready For The Big Day? – Clearwater Dentistry
Capturing the Moment At Andrew J. Holloman, DDS & Associates we know that just about anyone who has taken on
Dental Visits Are Not So Bad – Clearwater Dentistry
Many people dread going to the dentist. Dental visits have the reputation of being painful and uncomfortable, and it is
St. Patrick’s Day: Celtic Pride, Green Shamrocks, And Lucky Charms! – Clearwater Dentistry
“St. Patrick’s Day is an enchanted time — a day to begin transforming winter’s dreams into summer’s magic.” Adrienne Cook
Go Green For St. Patrick’s Day – Clearwater Dentistry
Millions of people, around Clearwater, FL and beyond, wear green on St. Patrick’s Day so they can show their spirit
Treatment Options To Improve Smile Symmetry – Clearwater Dentistry
One common reason for Cosmetic Dentistry treatment is to correct the look of an asymmetrical smile. You might have teeth that appear
What Makes A Prosthodontist Different From A Dentist? – Clearwater Dentistry
Many people are confused when it comes to which specialist they need to see about their dental needs. However, it
Are You At Risk For Oral Cancer? – Clearwater Dentistry
Nearly 40,000 people are diagnosed with oral cancer annually in the United States, with more than 8,000 dying every year
How Do I Overcome My Dental Anxiety? – Clearwater Dentistry
Do you feel anxious before every dentist appointment? If the answer is yes, you are not alone—more than 75 percent
What Exactly Is A Root Canal? – Clearwater Dentistry
Hearing that you need a root canal can be highly intimidating. What is a root canal? It is the removal
April Is Oral Cancer Awareness Month – Clearwater Dentistry
What is oral cancer? April is Oral Cancer Awareness Month. If you have been putting off a visit to our
April Is National Facial Protection Month – Clearwater Dentistry
The Importance of Facial Protection Americans from all walks of life should mark April as National Facial Protection Month on
Dental FAQs | Clearwater Dentistry | Florida Dentist
What is dentistry? Dentistry is the diagnosis, treatment, and prevention of conditions, disorders, and diseases of the teeth, gums, mouth,
Welcome To Our Blog – Clearwater Dentistry
Thank you for taking the time to visit our blog. Please check back often for weekly updates on fun
Three Must-Have Dental Treatments – Clearwater Dentistry
In dentistry, there are a wide variety of treatments, everything from elective procedures to those that are necessary and potentially
Understanding Cavities – Clearwater Dentistry
Getting a cavity seems like delayed punishment for eating that special dessert every weekend or for the few days you
Get Health Dental Tips From Clearwater FL Dentist
Are you doing everything possible to keep your smile in optimal shape? It makes sense to revisit your oral health
Every Day Is Earth Day – Clearwater Dentistry
During the early days of the environmental awareness movement, those who demonstrated against pollution, toxic chemicals, and the general public
Earth Day – Clearwater Dentistry
The idea for Earth Day was the brainchild of Gaylord Nelson, a senator from Wisconsin. He envisioned an Earth Day
Make Every Day Earth Day – Clearwater Dentistry
Earth Day began in 1970 as an event to raise awareness of our environment. What began as a single day
Are You A Tooth Grinder? – Clearwater Dentistry
Perhaps you had a particularly irritating commute home from work, and you realize at the end that your jaw was
Are You Nervous About Seeing The Dentist? You’re Not Alone! – Clearwater Dentistry
With advances in modern dentistry, a trip to Andrew J. Holloman, DDS & Associates these days is pretty routine. But
May Marks National Physical Fitness And Sports Month! – Clearwater Dentistry
The merry month of May also happens to be National Fitness and Sports Month, so take advantage of the warmer
Summer Is Almost Here: Tips For A Bright, White Smile! – Clearwater Dentistry
Summer is almost here, which means a season full of vacations, adventures and great memories is just around the corner
Wishing All Our Moms A Happy Mother’s Day! – Clearwater Dentistry
“Motherhood: All love begins and ends there.” – Robert Browning We would like to take this moment to thank all
Sleep Apnea: How We Can Help – Clearwater Dentistry
At Andrew J. Holloman, DDS & Associates, we understand that getting high-quality sleep is vital to maintaining your overall health.
Which Toothpaste Should I Use? – Clearwater Dentistry
Toothpastes come in many forms and boast different flavors, benefits, and endorsements. All are designed to remove surface bacteria and
Dental Infections – Clearwater Dentistry
Dr. Andrew Holloman and our team at Andrew J. Holloman, DDS & Associates will tell you that dental infections can
Heart Disease And Oral Health – Clearwater Dentistry
According to the National Institute of Dental and Craniofacial Research, more than 200 million Americans suffer from some degree of
Clearwater FL Dentist Offers Options For Gum Treatment
Irregular gums can ruin your smile – teeth can appear too large or too small; or you may suffer from
Memorial Day And Getting Ready For Summer – Clearwater Dentistry
Memorial Day didn’t become an official holiday until 1971, but Americans started gathering annually in the spring to remember those
Memorial Day – Clearwater Dentistry
Memorial Day is not only a federal holiday in the United States, but it is a day of observance and
Memorial Day: Parades, Remembrance, And The Unofficial Start Of Summer! – Clearwater Dentistry
“The purpose of all war is peace.” – Saint Augustine Fire truck sirens, baton twirlers, marching bands covering patriotic tunes,
Telltale Signs That Your Tooth Has A Cavity – Clearwater Dentistry
Dr. Andrew Holloman and our team at Andrew J. Holloman, DDS & Associates frequently get questions about cavity causes and
What To Look For When Choosing A Mouthwash – Clearwater Dentistry
Mouthwash is important for more than just keeping your breath fresh and smelling great. Combined with other forms of dental
My Gums Are Shrinking! – Clearwater Dentistry
Have you ever looked in the mirror and noticed that your teeth looked longer? Does it seem like your gums
Getting Ready For Summer Sports – Clearwater Dentistry
With the warmer and longer days here, we know many of our patients at Andrew J. Holloman, DDS & Associates
Summer Break: An Ideal Time For Wisdom Teeth Removal – Clearwater Dentistry
After your son or daughter departs for college, the last thing you want to get is a call or text
Are Dental Implants Right For YOU? – Clearwater Dentistry
Improve your health and quality of life with dental implants. Start eating the foods you love and living the life
June Is National Smile Month: Show Off Your Smile! – Clearwater Dentistry
The community health awareness group Oral Health America has reported that 82 percent of adults are unaware of the role
Early Detection Is Key To Treating Oral Cancer – Clearwater Dentistry
Every hour of every day, someone in North America dies of oral cancer, the sixth most common diagnosed form of
Is Your Child A Mouth Breather? – Clearwater Dentistry
Have you ever watched to see if your child is breathing through his or her mouth? Breathing through the mouth
What Should I Do If My Child Has A Toothache? – Clearwater Dentistry
Toothaches in children can be tricky ordeals that cause distress for both the child and the parent. You may feel
What Are Dental Crowns? – Clearwater Dentistry
A dental crown is often called a “cap.” A dental crown covers all of the visible parts of the tooth
I Drink A Lot Of Coffee. Could It Be Hurting My Smile? – Clearwater Dentistry
At Andrew J. Holloman, DDS & Associates, we know most of our patients enjoy a cup of coffee or two
The Success Of Dental Implants In Clearwater FL
Dental Implants provide an ideal solution when tooth loss is imminent or has already occurred. The patient’s overall health is reviewed
How Can A Prosthodontist Restore My Smile? – Clearwater Dentistry
Prosthodontics, or prosthetic dentistry, is an area of dentistry that concentrates on the aesthetic restoration and replacement of teeth to
What Are Dental Sealants And How Do They Work? – Clearwater Dentistry
A dental sealant is a liquid that is applied to the teeth. The sealant hardens and provides a protective coating
I’m On A Diet And Getting MORE Cavities! – Clearwater Dentistry
Health gurus rave about replacing unhealthy food choices with healthy ones in your diet. If you want to maintain your
Top Reasons People Choose Veneers – Clearwater Dentistry
Dental veneers are a way to correct and transform your smile by using “contact lens”-thin shells of porcelain or ceramic
Find Clearwater Dentist | Smile Brighter Now | Clearwater Dentistry
Find Clearwater Dentist | Smile Brighter Now Are you looking to find clear water Clearwater dentists will let you recommend
Happy Fourth Of July – Clearwater Dentistry
Every year, Americans all over the world celebrate the birth of the country and its independence on the Fourth of
Happy Fourth Of July! – Clearwater Dentistry
Happy Independence Day from Dr. Andrew Holloman and team! The Fourth of July celebrations in America may have changed a
Fun Facts For The Fourth – Clearwater Dentistry
The Fourth of July is a great time to get together with friends and family members for BBQ, games, fireworks,
Don’t Let A Dental Emergency Ruin Your Summer Vacation! – Clearwater Dentistry
For many of our patients at Andrew J. Holloman, DDS & Associates, summer means a season of relaxation, vacation, and
Teeth Grinding: Not Just A Bad Habit, But A Dental Concern – Clearwater Dentistry
Perhaps you don’t even know you grind your teeth. Maybe a spouse or loved one woke you up in the
Navigating The World Of Dental Insurance Terminology – Clearwater Dentistry
Unless you work for an insurance company, you probably do not spend a lot of your time studying all the
Canker Sores And Stress – Clearwater Dentistry
Canker sores are painful lesions that form in the soft tissues of the mouth, usually along the inner lips, under
Family Dentist In Clearwater FL Explains Importance Of Daily Flossing
When you brush your toothbrush only reaches two thirds of the surfaces of your teeth. Flossing removes what your toothbrush
Solutions For Dry Mouth (Xerostomia) – Clearwater Dentistry
Dry mouth, or xerostomia, is a common side effect of many medications. It can also be a side effect of
Antibiotic Prophylaxis Or Pre-Medication – Clearwater Dentistry
At Andrew J. Holloman, DDS & Associates, we know the human mouth contains a lot of bacteria. A bacterium can
How Do I Prevent Oral Cancer? – Clearwater Dentistry
The fact is, according to the Oral Cancer Foundation, close to 40,000 Americans will be diagnosed with oral or pharyngeal
What Is Hand-Foot-And-Mouth Disease? – Clearwater Dentistry
Hand-foot-and-mouth disease, or HFMD, is a type of contagious viral illness that causes a rash in the mouth and on
Five Tips For Taking Tots To The Dentist – Clearwater Dentistry
Toddlers are notoriously balky about strangers. But their first dental visit should not be cause for fear and tears. Nor
Women’s Hormones And Oral Health – Clearwater Dentistry
At Andrew J. Holloman, DDS & Associates, we know that hormones affect a woman’s mood, but did you know they
Alleviate Tooth Sensitivity – Clearwater Dentistry
If a sip of ice water, spoonful of ice cream, or piping hot latte is enough to send shivers up
How To Handle An Unexpected Dental Emergency – Clearwater Dentistry
Regardless of the type of dental emergency you experience, it is important that you visit Andrew J. Holloman, DDS &
Tooth Worms? The History Of Cavities And Tooth Fillings – Clearwater Dentistry
Scientists have discovered tooth decay in specimens that are more than 15,000 years old. The ancients once thought that cavities
When Was Your Last Dental Checkup? – Clearwater Dentistry
While Dr. Andrew Holloman and our team tell you daily oral hygiene habits, such as brushing and flossing, are essential
Clearwater FL Dentist Explains Benefits Of Sedation Dentistry
Are you apprehensive about visiting the dentist because you heard about someone else’s negative experience? Perhaps you dread dental appointments
Minimally Invasive Dentistry – Clearwater Dentistry
As the field of dentistry advances and the use of technology in the field increases, the concept of minimally invasive
Celebrate Labor Day By Getting Away – Clearwater Dentistry
Labor Day honors the contributions that workers have made to this country, and for many Americans, the holiday is a
Happy Labor Day! – Clearwater Dentistry
Labor Day is upon us, and that means the non-official end to summer. Before the kids head back to school
What Was Your Favorite Part Of Summer? – Clearwater Dentistry
It’s the end of summer, and fall is just around the corner. Soon the temperatures will cool down, the leaves
What Is Hyperdontia? – Clearwater Dentistry
When a child is born, he or she will have 20 primary teeth and 32 permanent teeth. But sometimes kids
Love Your New Smile? Tell Us About It! – Clearwater Dentistry
At Andrew J. Holloman, DDS & Associates, we have been creating beautiful smiles for years. Whether you have visited Dr.
Privacy Policy | Clearwater Dentistry
Clearwater Dentistry THIS IS A CONTRACT. PLEASE CAREFULLY READ THE FOLLOWING TERMS BEFORE ACCESSING THIS SITE. BY ACCESSING THE SITE,
How Do I Pick The Right Toothpaste For My Needs? – Clearwater Dentistry
With so many toothpastes available in so many price ranges, it can be difficult to be sure you are selecting
Steer Clear Of That Candy! – Clearwater Dentistry
At Andrew J. Holloman, DDS & Associates, we know how tempting candy can sometimes be on our sweet tooth, but
Gum Disease Symptoms | Andrew Holloman, DDS, Clearwater FL
Gum Disease is a serious disease that affects millions of people annually. Since it progresses in stages, people often do not
Do Adults Need Fluoride Treatments? – Clearwater Dentistry
Many dentists and hygienists recommend fluoride treatments for their adult patients. You might ask yourself, “Do I really need a
Common Emergency Care Visits: Toothaches Or Abscesses – Clearwater Dentistry
Dental problems do not always wait for normal office hours. Broken fillings or damaged teeth are common reasons for emergency
Oral Health Concerns For Infants – Clearwater Dentistry
Because babies’ teeth don’t appear until around six to eight months of age, it’s a natural misconception that they don’t
Care For Your Dentures – Clearwater Dentistry
Just like natural teeth, Dr. Andrew Holloman will tell you that dentures have a tendency to get coated with plaque,
October Is National Dental Hygiene Month: A Simple Oral Health Routine For Your Busy Lifestyle – Clearwater Dentistry
Adults are no strangers to feeling like there is never enough time in the day to get everything done. Your
Year-End Insurance Reminder – Clearwater Dentistry
Dr. Andrew Holloman, as well as our team at Andrew J. Holloman, DDS & Associates, would like to give those
Is Dairy Crucial To My Child’s Oral Health? – Clearwater Dentistry
Healthy eating, combined with regular physical activity, plays a vital role in your child’s health and well-being. Dairy foods are
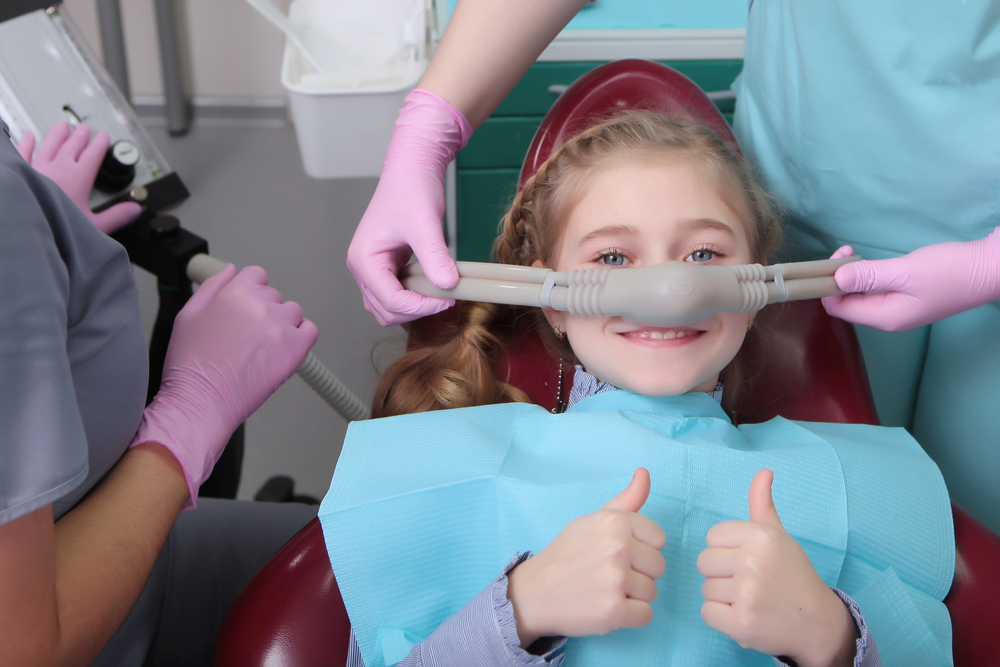
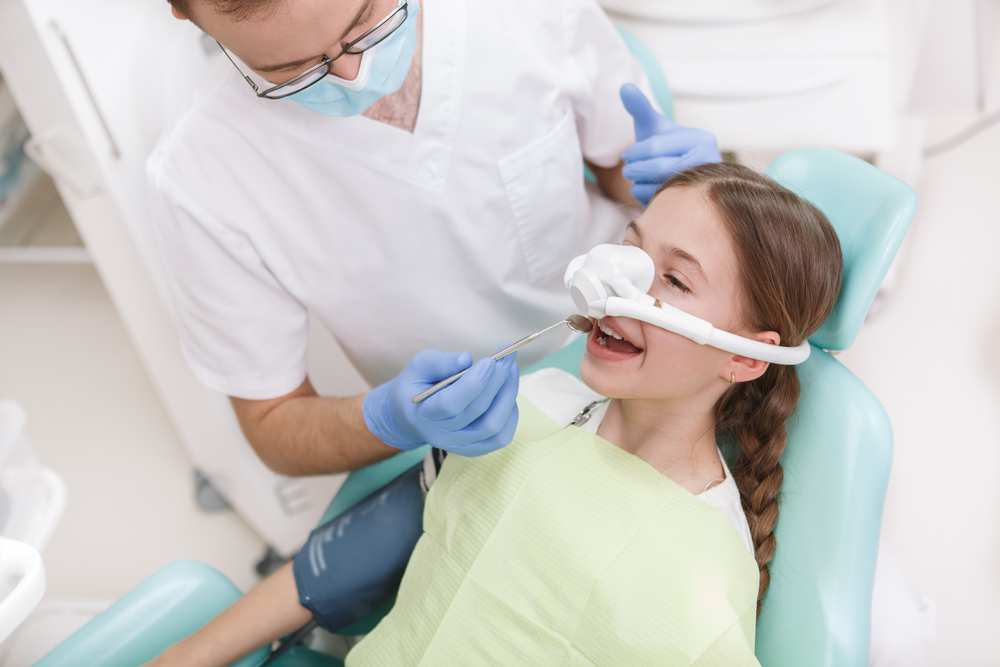
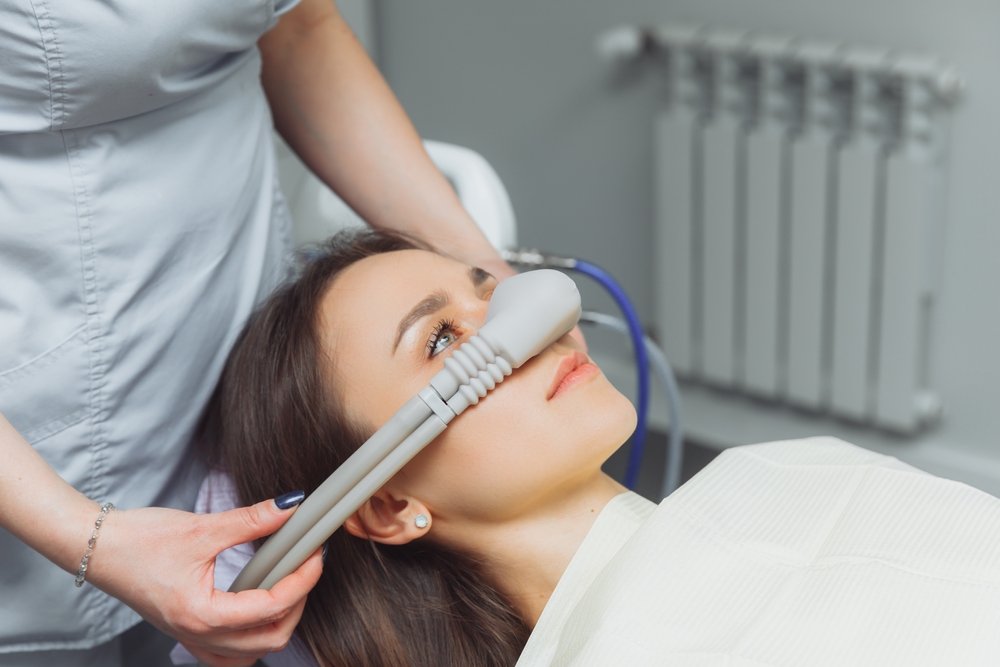
What Is Nitrous Oxide And Is It Safe? – Clearwater Dentistry
Our team at Andrew J. Holloman, DDS & Associates understands that the sights, sounds and sensations at a dental office
I Have Fluoride Toothpaste And Fluoridated Water; Do I Need A Fluoride Treatment? – Clearwater Dentistry
Fluoride is a naturally found ion with a history of greatly reducing the incidence of tooth decay in children. However,
It’s Been Years Since My Last Appointment; What Should I Expect? – Clearwater Dentistry
Feeling apprehensive or guilty for not visiting a dentist in over a year is common, but coming back to receive
Halloween: Candy, Costumes, And More! – Clearwater Dentistry
All Hallows’ Eve, more commonly known as Halloween, is a yearly event celebrated on October 31, and one that is
The Intriguing History Of Halloween – Clearwater Dentistry
Halloween is fast approaching, and Dr. Andrew Holloman wanted to be sure to wish our patients a happy day, no
November Marks National Diabetes Awareness Month – Clearwater Dentistry
Diabetes is a chronic disease that increases the risk for many serious health problems, including severe gum disease. November is
What Is A Water Pick And Do I Need One? – Clearwater Dentistry
Water picks, sometimes called “oral irrigators,” make an excellent addition to your regular home care regimen of brushing and flossing.
How Do I Know When I Have A Cavity? – Clearwater Dentistry
Dr. Andrew Holloman and our team at Andrew J. Holloman, DDS & Associates frequently field questions about cavities and what
Dental Veneers – Clearwater Dentistry
Are you looking to improve the appearance of your front teeth? Dental veneers are widely used to improve the appearance
Clearwater FL Dentist Offers Tips To Avoid A Dental Emergency
Your oral health is a complex and thriving system that is meant to last a lifetime. Unfortunately, accidents do happen,
A Holiday Recipe Favorite… Potato Casserole Supreme! – Clearwater Dentistry
This recipe yields 15 buffet servings; double as needed! Ingredients 5 pounds of potatoes (Yukon Gold or red-skinned) ½ cup
Top Five Ways To Improve Heart Health – Clearwater Dentistry
While there is no definite evidence that if your prevent gum diseases, like periodontitis, that you may be able to
Ten Fun Things To Do With Your Old Toothbrush – Clearwater Dentistry
Dr. Andrew Holloman and our staff recommend that you replace your worn-out, germy toothbrush with a new one every three
Thanksgiving – Clearwater Dentistry
At Andrew J. Holloman, DDS & Associates, we love to celebrate the holidays with vigor! Dr. Andrew Holloman would love
Clearwater FL Dentist Discusses Taking Care Of Dental Crowns
Dental Crowns have been used for decades to save teeth that have been cracked, broken, or suffered from severe dental decay.
Thanksgiving In North America – Clearwater Dentistry
Thanksgiving marks the start to the holidays; a season filled with feasting, indulging, and spending time with family and friends
What Are Implant-Supported Dentures? – Clearwater Dentistry
Great question. Implant-supported dentures are a great option for patients who are missing multiple teeth. Because they are secured by
Keep It Cheesy For A Long-Lasting Smile – Clearwater Dentistry
You’ve heard people tell you to say “cheese” when you’re having your picture taken, probably more times than you can
Implants: Why It’s Important To Replace Missing Teeth – Clearwater Dentistry
The average adult has 32 teeth, a combination of molars, canines, and incisors. By middle age, however, most adults are
Why Visiting The Emergency Room For Your Dental Problem Isn’t A Good Idea – Clearwater Dentistry
Emergency rooms are for emergencies, so before you head to the hospital because of a dental problem, you need to
Clearwater FL Dentist Explains When Dental Crowns Are Necessary
A dental crown can help to protect a tooth that has been severely damaged by decay or injury. It can
The Effects Of Biting Your Nails – Clearwater Dentistry
Also known as onchophagia, the habit of nail biting is one of the so-called “nervous habits” that can be triggered
What Type Of Toothpaste Is Right For You? – Clearwater Dentistry
Toothpaste no longer comes in simple choices of fluoride and fresh breath. Paste is not even the only option! You
Preventing Gum Disease At Clearwater FL Dentist
Gum Disease is a common and preventable cause of tooth loss in adults. In fact, it is the most common cause
Can My Child Really Avoid Tooth Decay? – Clearwater Dentistry
Great question! Yes, in fact, tooth decay is preventable! Decay, which is caused by sugars left in your child’s mouth,
Why Should I Have My Child’s Wisdom Teeth Removed? – Clearwater Dentistry
The wisdom teeth are the last of the permanent molars to emerge from the gums. This can occur as early
It’s A Wrap: Ending The Year With A Smile! – Clearwater Dentistry
People have been ushering in the New Year for centuries but it became an official holiday in 1582 when Pope
New Year’s Day Around The World – Clearwater Dentistry
New Year’s Day marks the beginning of the calendar year in most parts of the world. The holiday is celebrated
Candidates For Soft Tissue Or Bone Grafting
Soft tissue and bone grafting are not the most common or well-known dental procedures. Nevertheless, you may need them at
When Should I Start Bringing My Child In To The Dentist
Oral care is an important aspect of your child’s health. As a smart parent, you should know the right time
Tooth Extraction For Periodontal Disease
Studies show that periodontal disease is prevalent in many countries including the United States. The American Dental Association recognizes that
Clearwater FL Cosmetic Dentist Offers Teeth Whitening
Have you tried to whiten your smile with over the counter products and were disappointed with the results? Many people
It’s Been Years Since My Last Appointment; What Should I Expect? – Clearwater Dentistry
Feeling apprehensive or guilty for not visiting a dentist in over a year is common, but coming back to receive
November Marks National Diabetes Awareness Month – Clearwater Dentistry
Diabetes is a chronic disease that increases the risk for many serious health problems, including severe gum disease. November is
Implants: Why It’s Important To Replace Missing Teeth – Clearwater Dentistry
The average adult has 32 teeth, a combination of molars, canines, and incisors. By middle age, however, most adults are
Are You A Candidate For Dental Implants?
Dental implants have revolutionized the field of dentistry, providing a long-lasting and reliable solution for replacing missing teeth. These artificial
General Dentist In Clearwater FL
Our practice offers an array of general dentistry services to help members of our community establish and maintain great oral
Why Are Routine Pediatric Dental Exams Important?
The American Academy of Pediatric Dentistry recommends that all children attend routine pediatric dental exams twice each year as soon
Overcoming Dental Anxiety With Sedation Dentistry
If you experience extreme dread at the thought of visiting the dentist, you are not alone. Most people experience a
Am I A Candidate For Cosmetic Dental Bonding?
Do you suffer from an unsightly smile that you are embarrassed about or causes you to have self-esteem issues? The
Who Should Get Veneers?
Your smile plays a significant role in making the first impression. You may not be making a good impression if
5 Things You Can Do To Prevent Cavities
Everyone knows that excellent oral hygiene is the best way to keep teeth healthy and clean. However, cavities remain a